PSORIASIS
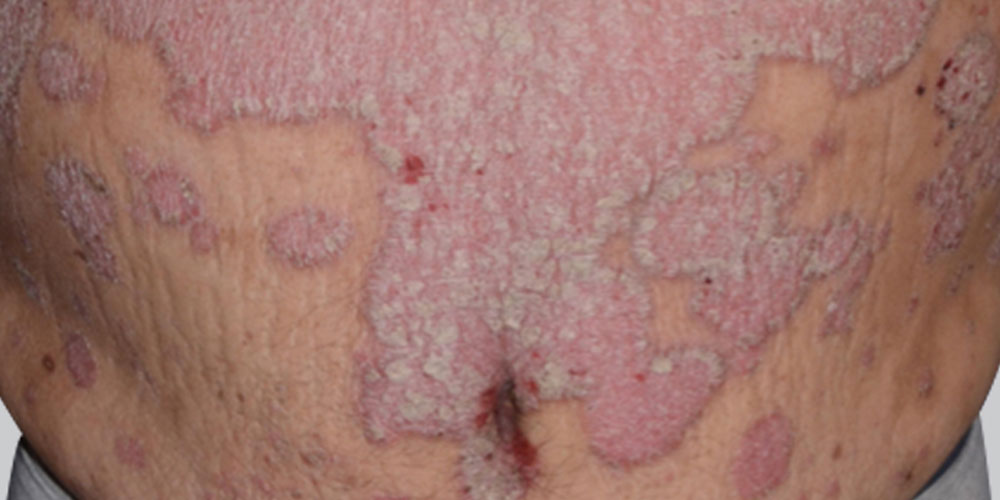

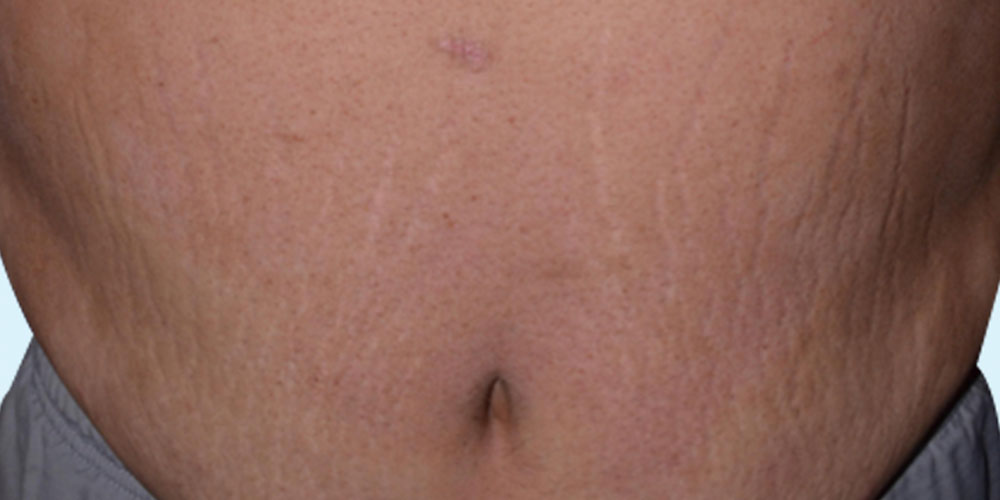
Psoriasis is a skin disease that causes red, itchy scaly patches, most commonly on the knees, elbows, trunk and scalp.
Psoriasis is a common, long-term (chronic) disease with no cure. It tends to go through cycles, flaring for a few weeks or months, then subsiding for a while or going into remission. Treatments are available to help you manage symptoms. And you can incorporate lifestyle habits and coping strategies to help you live better with psoriasis.
Psoriasis therapy is in the process of total transformation with the addition of new biological agents to the medication scene. With new FDA approval, we will be prepared to offer them to our patients, having prepared and studied well before their release.
WHAT IS PSORIASIS?
Psoriasis is a chronic skin condition affecting about 6 million people in the United States. Small or large round or oval red patches with thick white scales characterize it. These are sometimes itchy, occasionally hurt or bleed, or can be asymptomatic, except for the annoyance of shedding flakes of skin. The most common locations are elbows, knees and scalp, but it can occur on any part of the body. 5% of people with psoriasis also have arthritis. The onset of psoriasis can occur at any age including childhood and old age, although it most commonly appears in the teens-twenties. Sunlight tends to make it better for reasons explained below, whereas alcohol ingestion, lack of sunlight and stress tend to exacerbate it.
WHAT CAUSES PSORIASIS?
The cause of psoriasis isn’t completely known but it is now believed to be an autoimmune disease (a disease caused by one’s own immune system, leading it to attack one’s own otherwise normal tissues). Some part of the skin’s immune system is overactive and this leads to a sped up metabolism in the skin. Normal skin renews itself every 60 days; psoriatic skin only takes 9. Usually old, used up skin cells are shed so slowly we don’t notice it, but the increased turnover time in skin effected with psoriasis leads to the characteristic “shedding” of large flakes on a regular basis. There is also a genetic predisposition to it, although inheritance of psoriasis is complex. As many as 40% of people who have psoriasis report having no family history of the disease. This may be due to the fact that the genetics are complicated (more than one gene involved), there is incomplete expressivity of the genetic trait (not everyone who has the genetic makeup for psoriasis actually manifests the disease) or that the psoriasis in a family member was so mild as to go undiagnosed (e.g. a scaly scalp may have been mistaken for dandruff or a small patch on one elbow was ignored).
ARE THERE DIFFERENT TYPES OF PSORIASIS?
There are different types of psoriasis.
- Plaque type is the most common, with round to oval raised patches of scaly red skin.
- Guttate psoriasis refers to the abrupt onset of psoriasis in very small patches spread widely over the body. This typically occurs after being infected with a strep throat.
- Hand/foot psoriasis affects mainly hands and feet. Fingernails and toenails can be involved in any type of psoriasis resulting in pits, thickening and yellowish and brown discoloration.
- Erythrodermic psoriasis, which means the entire body, is covered with thin red scales.
- Pustular psoriasis which involves small pustules (bumps filled with pus) scattered about on the red plaques. Erythrodermic and pustular psoriasis are serious in that they can be accompanied by systemic symptoms such as fever and illness and sometimes require hospitalization, because the skin can’t retain enough body heat or fluids when effected in this way.
The severity is typically calculated on the percentage of body surface involvement. The % body surface is estimated on the “rule of 10’s”- each arm is 10%, each leg and each half of the torso is 20%, each hand or foot is 1% and the head is 6%. However, sometimes psoriasis is disabling by virtue of its location, even though the total body surface area is small; for instance, if it involves the hands in someone who requires fine manual dexterity in his/her profession.
It is estimated that about one-fifth of all individuals with psoriasis have more than a 20% body surface area involvement, thus making their psoriasis difficult to treat with topical medications and more appropriately treated with a total body type of therapy, whether ultraviolet light or a systemic medication.
WHAT DOES PSORIASIS LOOK LIKE?
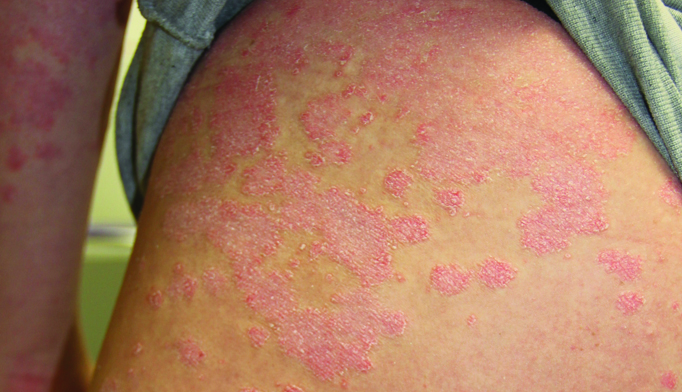
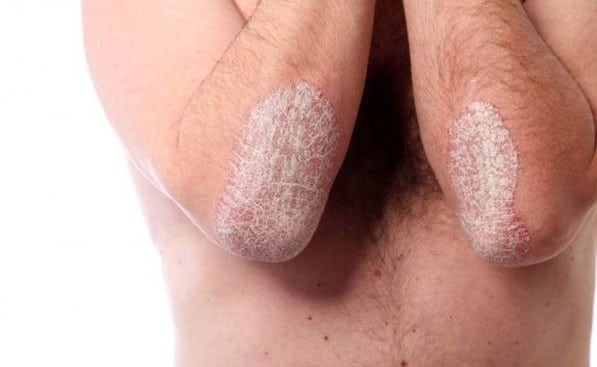
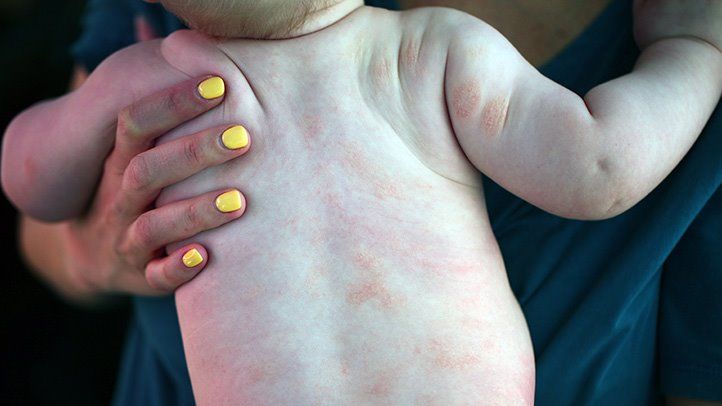
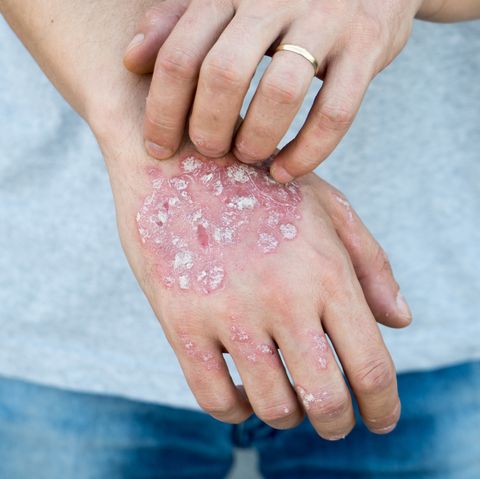
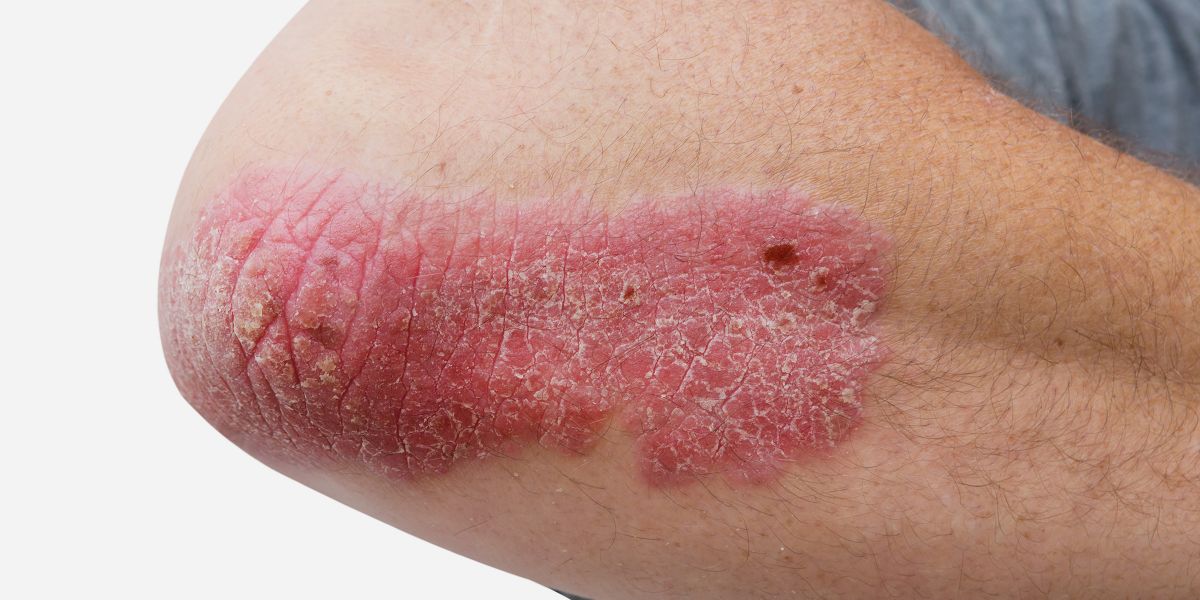
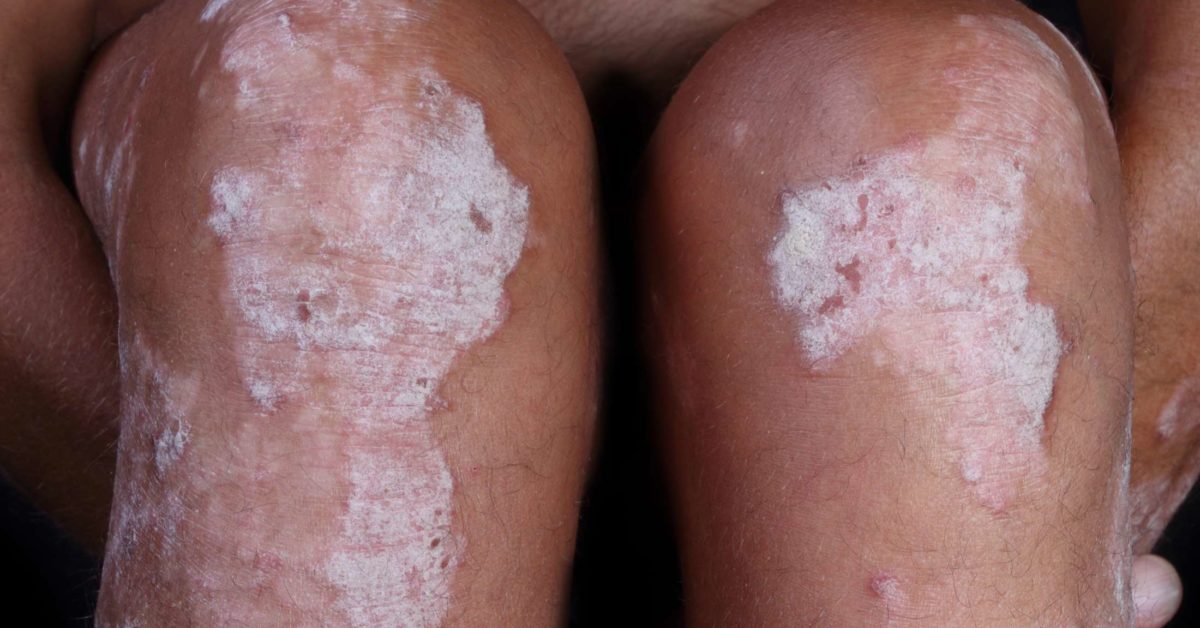
IS PSORIASIS CURABLE?
Psoriasis is a chronic disease. Chronic means it is long-term, i.e., lifelong as it is not curable. It has been demonstrated that having psoriasis significantly impacts the quality of life for those who suffer from it . The personal dissatisfaction associated with being afflicted with it is expressed by the phrase “the heartbreak of psoriasis”. In addition, it can sometimes be difficult to truly get psoriasis under control, even with adequate therapy. There may be some gender differences as well, as it appears that women may suffer more when afflicted, partly because more aggressive therapies are withheld due to their danger to a potential unborn fetus. Psoriasis severity tends to wax and wane naturally with time. It usually gets worse in the winter, presumable because ultraviolet light helps. It appears to also be negatively affected by cigarette smoking, alcohol consumption, stress and skin trauma (called Koebnerization- areas frequently rubbed or damaged can sometimes lead to plaques of psoriasis). It is best to find a compassionate dermatologist who will take the time to include you in the treatment decision making process. Keeping psoriasis at bay requires patience and persistence but usually is within reach if you have realistic expectations and expert help.
HOW CAN I TREAT PSORIASIS?
Treatment: topical, UV light, systemic The treatment of psoriasis partly depends on the location of the psoriasis and how much of the body surface is covered. In mild psoriasis (<10% of body surface covered) topical agents (creams, ointments, gels and lotions) are often employed first. These usually consist of tar preparations, topical steroids (Clobex, Vanos, clobetasol or betamethasone), retinoids (Tazorac) or vitamin D derivative preparations (Dovonex).
If the body surface area is too great or the topical agents haven’t worked, ultraviolet light treatments or systemic agents can be employed (either oral or injectable medications). Finally there are systemic agents (oral medicines) which are used for moderate to severe psoriasis, when it is impractical to use topical agents and light treatments have failed or are impractical. Moderate or severe psoriasis may requires combinations of more than one treatment.
Topical There are four categories of topical (cream, lotion, ointments or gels applied directly to the skin) therapy used for psoriasis: steroids, vitamin D derivatives, retinoids (vitamin A derivatives), and tar based.
The most common topical treatment of psoriasis is a topical steroid. These have anti-inflammatory properties and decrease the redness and scaling relatively quickly. Their main drawback is that psoriasis skin often develops a resistance to them- that is, they work at first but stop working after a while (called tachyphylaxis). Also, if you stop using them suddenly, psoriasis can flare up to a degree that is worse than its original condition (called rebound flare). The topical steroids are best used in conjunction with one of the newer topical medicines for the treatment of psoriasis, calcipotriene and tazarotene (see below).
Another important topical therapy is the vitamin D derivative, calcipotriene (Dovonex). The advantages to this therapy is that it has few, if any, long term side effects and does not “lose its potency” over time. The disadvantage is that it works slowly, and as monotherapy (only using this and no other treatment), it isn’t too effective. However, using Dovonex along with a potent topical steroid seems to increase the effectiveness of both.
A third important topical therapy is the retinoid tazarotene (Tazorac). This does a good job with thick plaques of psoriasis. Its main side effect is irritation so it is important to avoid getting it on the normal skin that surrounds the patch of psoriasis. Like Dovonex, it works best when paired with a topical steroid (applied at a different time of day) in order to decrease the irritation.
Tar preparations are often effective but they are smelly and messy. A tar-like substance, LCD can sometimes be effective. A pharmacist can combine these with a topical steroid (compounded) as well.
Ultraviolet treatments Typically you would receive ultraviolet treatments in a dermatologist’s office standing in a box that looks like a phone booth. These need to be administered by trained personnel in a dermatologist’s office as care must be taken to gradually increase the exposure time or else a sunburn reaction can ensue which can be severe. In addition, these treatments typically need to be given 2-3 times per week over a period of 2-3 months to obtain clearance in a case of moderate-severe psoriasis. Although inconvenient, these are highly effective treatments for psoriasis and have been approved by the FDA since the 1970’s. The main drawback besides the inconvenience is that there appears to be an increased risk of skin cancer over a long period of time with the treatments, particularly PUVA.
Systemic There are three main oral systemic medicines used for the treatment of psoriasis: acitretin (Soriatane), methotrexate and cyclosporine.
Acitretin (Soriatane) is a retinoid, that is, a member of a group of hormone molecules that have many different effects on tissues. In the case of psoriasis, it tends to modulate the tissue metabolism, thereby decreasing the rapidity with which psoriatic skin is made and helping to normalize it. It is taken once or twice a day, depending on the dosage, which is usually 25-50mg per day. This drug cannot be taken by women of childbearing. It is relatively safe but only moderately effective.
Methotrexate is an anticancer drug that works on psoriasis by decreasing metabolism in overactive cells. Given in much lower dosages than that used for cancer, it has a 40-year track record that has proven it to be effective, fairly well tolerated and relatively inexpensive as a treatment for psoriasis. It is taken orally on 1-2 days out of the week, so it is convenient. Its main drawback is that it can cause severe liver damage that can’t reliably be ascertained by blood tests. This means that intermittent liver biopsies are necessary to ensure safety. It can also cause anemia (especially in the initial stages of treatment), increased susceptibility to infection (immunosuppression), mouth or stomach ulcers and hair loss.
Cyclosporine is an immunosuppressive agent used principally in preventing the immune system of organ transplant patients from rejecting their transplanted organs. The discovery that it could treat psoriasis led to the idea that psoriasis was an autoimmune disease. It also is taken orally, usually in dosages ranging from 2.5-5 mg/kg (150-400 mg/day for average size adults). It is highly effective and probably works faster than any other anti-psoriasis medication available, so it is particularly suitable for people with very severe forms of psoriasis who need rapid improvement (e.g. those with pustular or erythrodermic psoriasis). Occasionally it is used to get severe psoriasis under control quickly and then to switch to another, potentially less toxic therapy. Long-term, low-dose therapy has also been advocated. The main problem with cyclosporine therapy is that is can cause hypertension (high blood pressure) and kidney damage. Most experts don’t recommend continuing this agent for more than one year at a time.
Biologic medications in psoriasis?
The adverse effects of systemic drugs and the frequent visits required for phototherapy have stimulated scientists to search for safer and more convenient ways to treat moderate to severe psoriasis. The search has led to the development of “biologic” medications, made from live materials. Four biologics—Amevive, Raptiva, Remicade, Humira and Enbrel—are cleared by the FDA for the treatment of moderate to severe psoriasis.
Unlike systemic drugs and phototherapy, biologics are “designer” drugs that attack specific molecular targets in the immune system. Keep in mind, however, that some of the biologics are new, and their long-term adverse effects are not known. The effects of biologics on pregnant women and fetuses are not known.
To understand how these drugs work, it is necessary to understand how the immune system works in psoriasis.
The immune system protects against disease by attacking foreign substances that enter the body. The immune system has many types of cells, such as T cells, which must be activated before they can function. In psoriasis, “memory” T cells are overactivated and this leads to the appearance of psoriatic lesions on the skin.
Also, the immune system has chemical messengers, such as tumor necrosis factor-alpha (TNF-alpha), which stimulate certain cells to cause inflammation. People with psoriasis have too much TNF-alpha in their skin and people with psoriatic arthritis have too much TNF-alpha in their joints. The excessive TNF-alpha causes inflammation, which damages tissues and joints. TNF-alpha also leads to unwanted activation of T cells and the development of psoriasis.
Both Amevive (generic alefacept) and Raptiva (generic efalizumab) work by blocking the activation of T cells and the migration of these activated cells to the skin. The symptoms of many people with psoriasis improve when they take these drugs. Amevive is injected weekly as an intramuscular injection (into the buttock or the arm). Raptiva is self-injected under the skin once per week. Both require some monitoring via blood work.
Enbrel (generic etanercept), Remicade (generic infliximab), and Humira (generic adalimumab) work by reducing the amount of TNF-alpha in the skin and joints. This interferes with the inflammatory process and the development of psoriatic arthritis and psoriasis. Both Enbrel and Humira are self-injected, once or twice per week or every other week respectively. Remicade is an intravenous infusion which must be administered in the office of a doctor experienced with infusions.
Since these drugs affects the immune system, people with a high risk of cancer or frequent infections should not take the drug. Also, people taking TNF inhibitors need to be pre-screened for tuburculosis. Women who are pregnant and persons with a history of neurologic disease or heart disease should use these drugs with caution. This is a small and incomplete list of side effects. Before beginning a medication such as this you would need to consult thoroughly with your doctor.
SCHEDULE AN APPOINTMENT TODAY
ADDRESS
711 E Lamar Blvd # 200
Arlington, TX 76011
moreinfo@acderm.com
PHONE
817-795-SKIN (7546)
HOURS
Mon – Thur | 7:00 AM – 4:00 PM
Fri | 07:00 AM – 12:00 PM
Closed on Weekends
GO WITH CONFIDENCE
How can I find out more?
American Academy of Dermatology (AAD) 930 N. Meachum Road Schaumburg, IL 60173 888-462-DERM www.aad.org
National Psoriasis Foundation 6600 SW 92nd, Suite 300 Portland, OR 97223-7915 800-723-9166 www.psoriasis.org
Where did this information come from?
Ortonne JP. Recent developments in the understanding of the pathogenesis of psoriasis. Br J Dermatol 1999 Apr;140 Suppl 54:1-7.
Bagel J. Establishing a practical and effective psoriasis treatment center. Dermatol Clin 2000 Apr; 18 (2) : 349-57,xi.
Koo J. Systemic sequential therapy of psoriasis: a new paradigm for improved therapeutic results. J Am Acad Dermatol 1999 Sep;41(3 Pt 2):S25-8.
Shupack J, Abel E, Bauer E, Brown M, et al. Cyclosporine as maintenance therapy in patients with severe psoriasis. J Am Acad Dermatol 1997 Mar;36 (3 Pt. 1):423-32.
Rapp SR, Feldman SR Exum ML, Fleischer AB, et al. Psoriasis causes as much disability as other major medical diseases. J Am Acad Dermatol 1999 Sep;41 (3 Pt 1):401-7.
Al-Suwaiden SN, Feldman SR. Clearance is not a realistic expectation of psoriasis treatment. J Am Acad Dermatol 2000 May;42 (5 Pt.1) :796-802.
Hotard RS, Feldman SR, Fleischer AB. Sex-specific differences in the treatment of severe psoriasis. J Am Acad Dermatol 2000 Apr;42(4):620-623.
Higgins E. Alcohol, smoking and psoriasis. Clin Exp Dermatol 2000 Mar;25(2) :107-10.
Zachariae R, Oster H, Bjerring P, Kragballe K. Effects of psychological intervention on psoriasis: A preliminary report. J Am Acad Dermatol 1996;34:1008-15.







