What Do Poison Ivy Plants Look Like?
Poison Ivy is not the only cause of painful skin irritations. Poison ivy happens to be the only one major irritant plants that always has three leaves, one on each side and one in the center. Poison Ivy leaves are shiny with smooth or slightly notched edges. Poison Oak looks similar, but the leaves are larger and more rounded like an oak leaf. They have a textured, hairy surface. There may be groups of three, five, or seven leaves. Poison Sumac leaves grow in clusters of seven to 13 leaves, with one by itself at the end.
Where Does Poison Ivy Grow?
Poison ivy, oak, and sumac grow in wooded or marshy areas throughout the US. They have a sticky, long-lasting oil called urushiol that causes an itchy, blistering rash after it touches your skin. Even slight contact, like brushing up against the leaves, can leave the oil behind. Poison ivy and poison oak grow as vines or shrubs. Poison sumac is a shrub or tree.
What Should I Do If I Touch Poison Ivy?
Acting quickly after touching poison ivy, oak, or sumac may save you much pain and discomfort. You may be able to avoid a poison ivy rash or a poison oak rash or lessen its effect by washing your skin with a poison plant wash and then rinsing thoroughly. Immediately wash the part of your skin that touched the plant with one of the following: Rubbing alcohol, Poison ivy wash (cleanser, soap, or towelettes), Dishwashing soap, or Laundry detergent. Wash your skin gently. Scrubbing can cause a rash because you rub the plant’s oil, which is what leads to a rash, into your skin. Thoroughly rinse with plenty of cool water. This removes the rubbing alcohol or other product from your skin. Leaving one of these products on your skin could irritate your skin, causing a different type of rash. Also be sure to wash under your nails. This will remove any oil that may have gotten trapped there.
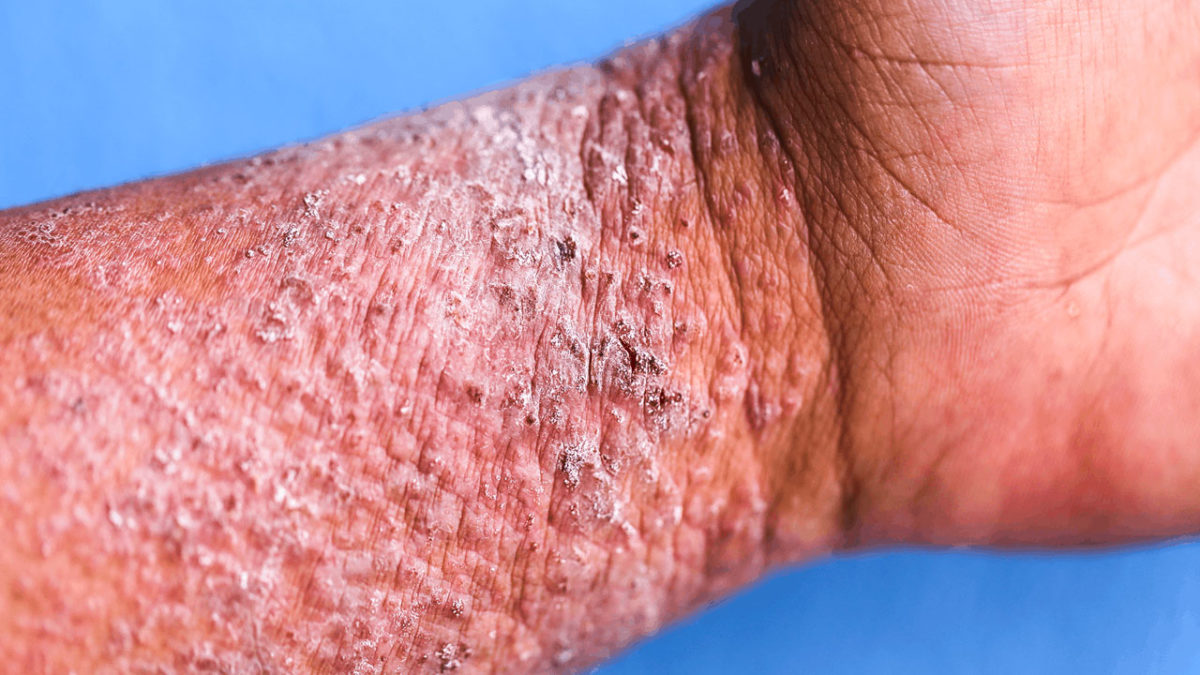
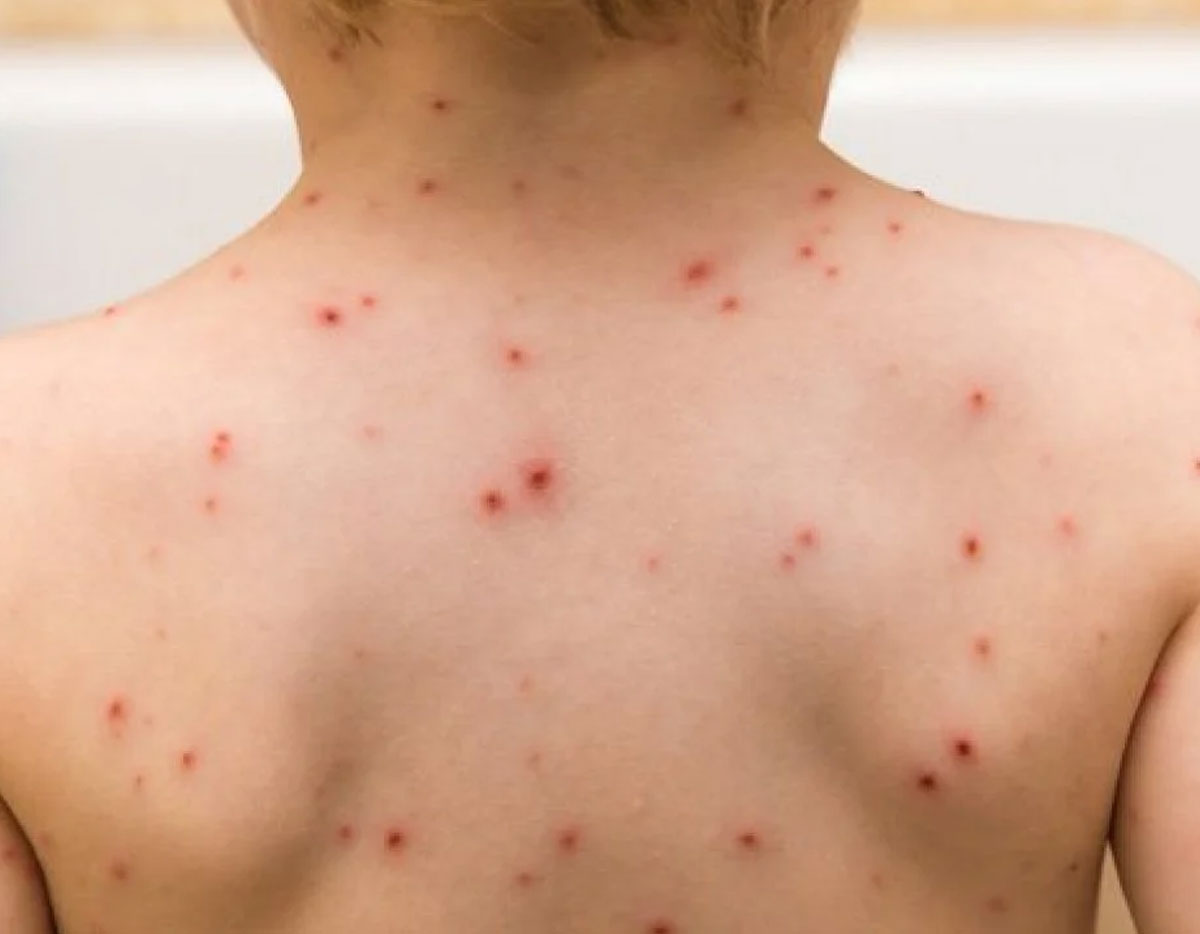
What Does The Rash Look Like?
It may take some time for the rash to appear. A rash can develop in a few hours if you’ve had a rash from one of these plants before. If you’ve never had a rash from poison ivy, oak, or sumac, it can take 2 to 3 weeks before you see a rash. The skin usually itches intensely where the rash will appear. The itch can be so intense that it wakes you from a sound sleep. Shortly after your skin starts to itch, the rash appears. Most people develop an itchy, red, and blistering rash. If you have blisters, they break open and leak fluid. The blisters crust over, and the rash clears in 2 to 3 weeks. The rash will clear without treatment, but it can be extremely itchy until it clears completely.
Why Does The Rash Seem to Spread?
While it may look like the rash is spreading, what’s most likely happening is that you’re developing one or more new rashes. This happens because the urushiol (the oil from these plants that causes the rash) came in contact with more than one area of your skin. Typically, the skin with the most oil on it develops a rash first. Skin with less oil tends to react later. Many people also mistakenly believe that when they touch their rash, they can spread the rash from one part of their body to another. You cannot spread the rash. Sometimes you can spread the oil causing the rash. Your skin absorbs the oil quickly, so you can only spread the oil from one part of your skin to another for a short amount of time.
How Long Does a Rash Last?
For people who have had previous rashes from poison ivy, the current rash tends to last 1 to 14 days before it clears on its own. Those who have never had the rash before may have a rash last for 21 days or longer before it goes away. The rash is not contagious, but the oil causing the rash can be spread to others if not washed away quickly. The oil can also be spread by clothing, pets or working utensils such as rakes and shovels.
How Can I Treat Poison Ivy Rash?
If you have any of the following, go to the emergency room immediately:
- Difficulty breathing or swallowing
- A rash around one or both eyes, your mouth, or on your genitals
- Swelling on your face, especially if an eye swells shut
- Itching that worsens or makes it impossible to sleep
- Rashes on most of your body
- A fever
These are signs of a severe reaction that require immediate medical care.
You can treat the rash at home if you:
- Have a mild rash
- Developed a rash on a small section of skin
- Are certain that the rash is due to poison ivy, oak, or sumac
For poison ivy treatment, immediately rinse your skin with lukewarm, soapy water. If you can rinse your skin immediately after touching poison ivy, poison oak, or poison sumac, you may be able to rinse off some of the oil. If not washed off, the oil can spread from person to person and to other areas of your body. Wash your clothing. Thoroughly wash all of the clothes you were wearing when you came into contact with the poisonous plant. The oil can stick to clothing, and if it touches your skin, it can cause another rash.
Do not scratch, as scratching can cause an infection. Leave blisters alone. If blisters open, do not remove the overlying skin, as the skin can protect the raw wound underneath and prevent infection.
What Can I Do To Relieve The Itch?
Take short, lukewarm baths. To ease the itch, take short, lukewarm baths in a colloidal oatmeal preparation, which you can buy at your local drugstore. You can also draw a bath and add one cup of baking soda to the running water. Taking short, cool showers may also help.
Use calamine lotion or hydrocortisone cream. Calamine lotion can reduce the itch. If you have a mild case, a hydrocortisone cream or lotion is another treatment that can alleviate the itch.
Apply cool compresses to the itchy skin. You can make a cool compress by wetting a clean washcloth with cold water and wringing it out so that it does not drip. Then, apply the cool cloth to the itchy skin.
Consider taking antihistamine pills. These pills can help reduce itching. You should not apply an antihistamine to your skin, as doing so can worsen the rash and the itch.
If your rash is not improving after 7 to 10 days, or you think your rash may be infected, see a board-certified dermatologist. A dermatologist can treat your rash and any infection and help relieve the itch.
Dermatologists emphasize that you only treat the rash if you’re absolutely certain that poison ivy, oak, or sumac caused it. If you’ve never had a poison ivy rash, see a doctor for a diagnosis.
Source https://www.aad.org/public/everyday-care/itchy-skin/poison-ivy